Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
Advertisement
You can also search for this author in PubMed Google Scholar
You have full access to this article via your institution.
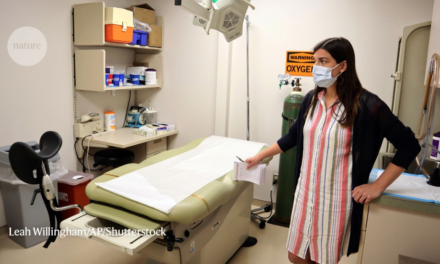
The World Health Organization’s director-general, Tedros Adhanom Ghebreyesus, rang the agency’s highest alarm on 23 July to signal the seriousness of the global monkeypox outbreaks.Credit: Lindsay Mackenzie/WHO
Over the weekend, the World Health Organization (WHO) declared that the monkeypox outbreak spreading globally is a ‘public health emergency of international concern’ (PHEIC). Researchers hope that the declaration — the agency’s highest alarm — might serve as a wake-up call for countries as they struggle to contain the spread of the virus that causes monkeypox.
Monkeypox vaccination begins — can the global outbreaks be contained?
Since the first cases were detected outside Africa in May, more than 16,500 people have been confirmed infected in nearly 80 countries that don’t typically see cases. Monkeypox has been circulating in parts of Africa for decades.
This is the seventh time since the alarm system originated in 2005 that the WHO has declared a PHEIC — a step it reserves for events that pose a risk to multiple countries, and that require a coordinated international response (see ‘The highest alarm’). Two of those warnings, for COVID-19 and polio, are still in place.
In an unprecedented move, WHO director-general Tedros Adhanom Ghebreyesus declared the PHEIC on 23 July, after a panel of advisers failed to come to a consensus. Although the panel doesn’t formally vote, six members were in favour of declaring a PHEIC, while nine were against, Tedros said at a press conference announcing his decision. The panel had previously met in late June, but at that time only three members were for declaring a PHEIC and 11 were opposed, so Tedros decided against sounding the alarm at the time.
The WHO has declared a ‘Public Health Emergency of International Concern,’ or PHEIC, seven times since the alarm system originated in 2005.
2009: H1N1 (swine flu) originates in Mexico and spreads to the United States.
2014: Polio resurges in Afghanistan, Pakistan and Nigeria.
2014: Ebola virus infections spread throughout Guinea, Sierra Leone and Liberia.
2016: A Zika virus epidemic causes microcephaly and other neurological disorders in the Americas.
2019: An Ebola outbreak spreads in a conflict zone in the Democratic Republic of the Congo.
2020: The first cases of COVID-19 appear in China in late 2019, and the SARS-CoV-2 coronavirus spreads to many other countries, becoming a pandemic.
2022: Monkeypox infections pop up and spread widely in countries outside Central and West Africa, where they had been slowly circulating for 50 years.
Source: This timeline was repurposed from this story, by Amy Maxmen.
Declaring the monkeypox outbreak a global emergency is a good decision, says Anne Rimoin, an epidemiologist at the University of California, Los Angeles, who is a member of the panel and has studied monkeypox in the Democratic Republic of the Congo for more than a decade. “It sends the right message, and it will hopefully mobilize attention and resources to prevent this virus from gaining a foothold globally.”
Researchers have been warning that the window of opportunity for containing the global monkeypox outbreak is rapidly closing. The virus is already established in an animal reservoir in some parts of Africa, making its eradication a difficult task. One fear is that the virus could spread from humans to animals elsewhere in the world, establishing further reservoirs from which humans could be infected repeatedly.
Monkeypox in Africa: the science the world ignored
Even as cases are soaring in Germany, Spain and the United States, some think that containment is still possible, however. The PHEIC signals loudly to public-health officials that the time to act is now, says Caitlin Rivers, an epidemiologist at Johns Hopkins University in Baltimore, Maryland. “We can’t accept this as an endemic virus,” she says.
Countries should work to increase the number of people tested, boost contact-tracing efforts and isolate people as early as possible after symptoms are detected, Rivers adds.
The PHEIC sends a clear message to countries that their participation in the global response — which might include sharing vaccines and treatments — is necessary for containment. The WHO issued guidelines for countries when announcing the alarm, offering recommendations on testing, public-health measures and messaging, travel advisories, infection prevention and control, and global coordination.
Wealthy countries have raced to deploy smallpox vaccines, thought to be highly effective against monkeypox because the viruses that cause these diseases are related. Although some children and women have been infected with monkeypox, almost all the infections in the global outbreak have occurred so far in men who have sex with men (MSM), especially those with multiple sexual partners. This has led public-health officials to focus their messaging and vaccine stockpiles on this population. At first, some countries, such as Canada and the United Kingdom, used a ‘ring vaccination’ approach, which inoculates the close contacts of people infected with monkeypox to cut off routes of transmission. They then moved quickly to offer the vaccine more widely to high-risk communities, including MSM and health-care workers.
Monkeypox outbreaks: 4 key questions researchers have
Researchers know that monkeypox spreads mainly through close contact. They are still investigating whether the virus can be sexually transmitted, but it has clearly taken hold in the MSM community. Some members of the WHO panel were reluctant to support a PHEIC declaration because they worried that it would stigmatize that community and hinder efforts to contain the virus. “People are not always willing to disclose sexual history”, especially in countries where homosexuality is criminalized, says Boghuma Titanji, an infectious-disease physician at Emory University in Atlanta, Georgia.
While wealthy countries use vaccines for monkeypox, Titanji warns that the ongoing outbreaks in Africa, where there have been more than 70 suspected deaths from the virus this year, “cannot be relegated to a footnote”. (So far, no deaths have occurred in people infected outside Africa.) She hopes that the WHO will promote equity in the global monkeypox response by helping to scale-up surveillance and testing for the virus in Africa, and by allocating money for research and vaccines there. “We got into this problem by allowing monkeypox to rage on for 50 years in Africa,” she says.
doi: https://doi.org/10.1038/d41586-022-02054-7
Editorial 09 AUG 22
News Feature 02 AUG 22
News 01 AUG 22
Editorial 03 AUG 22
News 26 JUL 22
Research Highlight 19 JUL 22
Career Feature 04 AUG 22
News 02 AUG 22
News 28 JUL 22
University of California Davis (UC Davis)
Davis, CA, United States
University of California Davis (UC Davis)
Davis, CA, United States
Stanford University
Stanford, CA, United States
Stanford School of Medicine
Stanford, CA, United States
You have full access to this article via your institution.
An essential round-up of science news, opinion and analysis, delivered to your inbox every weekday.
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
Advanced search
© 2022 Springer Nature Limited